ABSTRACT
Several risk factors including hypertension are common complications of pregnancy with preeclampsia particularly associated with substantial risk to both the mother and fetus. This cross-sectional study involving quantitative approach was conducted in Same District Hospital in Tanzania. Data were collected from all pregnant women in the hospital using questionnaires. Respondents’ knowledge on maternal mortality regarding preeclampsia included those who had no knowledge 60(60%), and those who had knowledge 40(40%). Most of the respondents had no knowledge of maternal mortality due to the complications of preeclampsia. The study revealed that 64(64%), had positive attitude towards maternal mortality due to preeclampsia prevention while 36(36%) had no response. About 68(68%) of the respondents could not access the health facilities saying that these health facilities were not affordable citing that the distance was too long. They reported no health facilities and services as well as insecurity while looking for health facilities/services and finally that there were few health workers in the health facilities meaning that patients could not be attended to on time. Furthermore, health workers harassed the patients and make them seek other alternatives when they are sick, while minority 32(32%) said that the health facilities were accessible, affordable and efficient. Medical history during prenatal care showed that 25% of the respondent had increased blood pressure more than 140/90 mmHg, but only 10% had breath issues. Laboratory diagnosis of the respondents revealed increased proteinuria (48%) and impaired liver function (7%). Respondents experienced 39% convulsion and 24% pulmonary edema. Overall, the study identified a few predisposing factors to preeclampsia/eclampsia among pregnant women. Also, most of the respondents were said to have no knowledge of eclampsia thereby increasing maternal mortality.
Key words: Preeclampsia, hemolytic elevated liver enzymes, eclampsia, low platelet count, disseminated intravascular coagulopathy, intrauterine growth restriction, intrauterine fetal death, pregnancy induced hypertension.
Hypertension is a common complication of pregnancy. Preeclampsia, in particular, is associated with substantial risk to both the mother and the fetus. Several risk factors have been recognized to predict risk for preeclampsia (Solomon and Seely, 2011). However, at present no biomarkers have sufficient discriminatory ability to be useful in clinical practice, and no effective preventive strategies have yet been identified (Solomon and Seely, 2011). Commonly used medications for the treatment of hypertension in pregnancy include methyldopa and labetalol. Blood pressure thresholds for initiating antihypertensive therapy are higher than outside of pregnancy. Women with prior preeclampsia are at increased risk of hypertension, cardiovascular disease, and renal disease (Suzuki et al., 2015). Pregnancy induced hypertension (PIH) is classified according to the severity of hypertension. The Japan society of hypertension made practice guidelines in 2014, and the Japan Society for the study of hypertension in pregnancy made its guidelines subsequently in 2015. Both guidelines stated that the basic treatment for PIH is the interruption of pregnancy, and antihypertensive therapy should be given for protection in the mother complicated by severe hypertension (Suzuki et al., 2015).
The fetal heart rates should be monitored enough due to worsening fetal circulation. It recommends that methyldopa, hydralazine, labetalol, and long-acting nifedipine (only after 20 weeks of gestation) should be used as the first-choice antihypertensive oral drugs. Intravenous administration should be selected when a hypertensive emergency occurs (Suzuki et al., 2015). Pregnancy-induced hypertension (PIH) complicates 6-10% of pregnancies around the world (WHO, 2011). However, hypertension and proteinuria which exist in preeclampsia, are present in 2-8% of all pregnancies (Steegers et al., 2010). In African countries such as South Africa, Egypt, Ethiopia and Tanzania, the rates of preeclampsia have been reported to vary from 1.8% to 7.1% (Osungbade and Ige, 2011).PIH is defined as systolic blood pressure (SBP) > 140 mmHg and diastolic blood pressure (DBP) > 90 mmHg. It is classified as mild (SBP 140-149 and DBP 90-99 mmHg), moderate (SBP 150-159 and DBP 100- 109 mmHg) and severe (SBP ≥160 and DBP ≥110 mmHg) (Kintiraki et al., 2015).
PIH refers to one of four conditions: a) pre-existing hypertension, b) gestational hypertension and preeclampsia (PE), c) pre-existing hypertension plus superimposed gestational hypertension with proteinuria and d) unclassifiable hypertension. PIH is a major cause of maternal, fetal and newborn morbidity and mortality. Women with PIH are at a greater risk of abruption placentae, cerebrovascular events, organ failure and disseminated intravascular coagulation (Kintiraki et al., 2015). Treatment of PIH depends on blood pressure levels, gestational age, presence of symptoms and associated risk factors. Non-drug management is recommended when SBP ranges between 140-149 mmHg or DBP between 90-99 mmHg. Blood pressure thresholds for drug management in pregnancy vary between different health’s organizations (Katon et al., 2012). There are many theories on the pathogenesis of preeclampsia, although the exact cause is not known. Most involve abnormal development of the
placenta, which leads to a distressed placenta that secretes factors into the maternal blood.
Maternal response (endothelial activation, pressor response, vasospasm) to these factors eventually leads to
high blood pressure and proteinuria (protein in the urine) generally after 20th
weeks of gestation (De Vera and Berard, 2012). Placenta is definitely the source of problem, and not the fetus. This is evident from preeclampsia happening in
molar pregnancy (
Hydatidiform Mole) which does not have foetal tissue. Preeclampsia can occur in extrauterine (for example abdominal) pregnancy which brings into question role of the maternal part (decidua) of the placenta. Preeclampsia is relieved on
parturition (delivery) or on
termination of pregnancy as the cause, that is the placenta, is removed. The maternal response reverts back to complete normal within a few months of delivery (Veerbeek et al., 2015). Women with pregnancy-induced hypertension have been noted to have an increased responsiveness to a variety of endogenous substances (prostaglandins, thromboxane) that can cause vasospasm and platelet aggregation.
Thrombus formation or hemorrhage affects the central nervous system leading to headache, local neurological deficits, and seizure. Renal necrosis leads to a decreased glomerular filtration rate and proteinuria. Liver injury from hepatocellular necrosis causes right upper quadrant pain and elevated liver function tests (Sajith et al., 2014). Cardiovascular manifestations include a lower than normal intravascular volume, increased cardiac output, and an abnormally elevated peripheral vascular resistance. Microangiopathic hemolysis leads to anemia and thrombocytopenia. Placental infarction and abruptio placentae lead to intrauterine growth retardation and fetal death (Vest and Cho, 2014). Preeclampsia typically involves a wide spectrum of clinical signs and symptoms. Mild preeclampsia is characterized by mild hypertension with no evidence of end-organ pathology aside from minimal proteinuria (<2.0 g/d) (van Middendorp et al., 2013). Severe preeclampsia is at the other end of the spectrum and is characterized by significant hypertension, more pronounced proteinuria (>5.0 g/d), and evidence of end- organ damage due to systemic vasoconstriction.
Severe preeclampsia can later lead to eclampsia which is the most dangerous condition to maternal and fetal well-being (Pieper et al., 2014). The most successful treatment for advancing preeclampsia or eclampsia is
delivery, either by
induction or
Caesarean section. Some forms of preeclampsia can be treated with anti-hypertensive medication. In some cases, women with preeclampsia or eclampsia can be stabilized temporarily with
magnesium sulfate intravenously to prevent seizures. Attempts will be made to delay delivery until the fetus has matured, but in severe cases where the mother's life is threatened, delivery must occur as soon as possible (Aghamohammadi et al., 2011). Preeclampsia occurs in about 6% of the general population. It is one of the life threatening conditions that affect pregnant women. Among the predisposing factors are black race, prim gravidity, change of paternity, preexisting hypertension and previous history of preeclampsia.
This condition can be complicated and leads to eclampsia, which is mostly fatal to the fetus as well as the mother. Other complications posed by this condition include abruptio placenta, disseminated intravascular coagulopathy, acute tubular necrosis, and thrombocytopenia to the maternal side. About 25-30% prematurity cases result from this condition. Also, 10-15% reduction in gestational age and intrapartum fetal distress result from this same condition. It is a third leading cause of maternal mortality worldwide. Owing to the fact that pregnant women are vulnerable to preeclampsia/eclampsia and its associated complications, then it follows that proper community understanding may lead to early detection of pregnancy risk and hence early booking and proper follow-up to reduce the complications associated with PIH/eclampsia. This concept formed the basis for this study to determine knowledge, the prevalence and risk factors associated with preeclampsia/eclampsia among pregnant women admitted at the maternity ward of Same District Hospital in Tanzania.
Study design
The study is a cross-sectional type involving quantitative approaches.
Site
The study area was Same District hospital in Tanzania.
Population
The study population included all pregnant women in the hospital.
Data collection
Data was collected using questionnaires.
Sample size determination
A sample size of 100 was used; this was determined using the following formula as previously explained (Daniel, 1999).
n = desired sample size; Z = Standard normal deviation usually set at 1.96; p = the proportion of study population that are at risk of preeclampsia (7%) (Osungbade and Ige, 2011); q = 1-p; d -= amount of error (0.05 levels).
By substitution
Data collection and processing
Data was collected using questionnaires which had both open ended and closed ended questions. The data was then entered into the computer by using Microsoft office word and Microsoft office Excel spreadsheets. The results were analyzed using SPSS Version 20.0.
Data analysis
Data was analyzed by using the SPSS and Microsoft office Excel Spreadsheets.
Data presentation
The data analyzed was presented by using tables, graphs, charts and texts together with interpretation of the research results
Ethical consideration
Ethical clearance for using human subjects was obtained from the Research Director of Same district. Permission was sought from the authorities to conduct the study in the area needed for the study. The purpose of the study was clearly explained to them.
Biodata
Age of respondents
According to Table 1, most of the respondents were aged between 25-34 (48%), followed by the age range of 35-44 (24%), and those aged between 45-49 (16%) of the total respondents. The young mothers were within the age range of 15-24 (12%).
Occupation of the respondent
Most of the respondents were peasants (65, 65%), followed by 19 (19%) who were self-employed and 16 (16%) that were civil servants (Figure 1).
Distance from nearest health facilities
According to Table 2, most of the respondents (48, 48%) covered a long distance of more than 10 km to the nearest health facilities, followed by 36 (36%) who covered 5 to 10 km and lastly 16 (16%) who covered less than 5 km.
Marital status
From the findings, most of the respondents were young and single (46, 46%), followed by the married (17, 17%), the engaged (27, 27%), the widowed (6, 6%) and finally those who separated from their partners 4 (4%) (Figure 2).
Religion of respondents
Majority of the respondent by religion (74, 74%) were Christians while the minority (26, 26%) were Muslims (Figure 3).
Level of education
Table 3 shows that the majority of the respondents (60, 60%) had primary status of education, 24 (24%) had no formal education, 12 (12%) had secondary form of education and finally 4(4%), had tertiary education.
Knowledge of preeclampsia
Table 4 shows the respondents' knowledge on preeclampsia. Those who had no knowledge were 60 (60%) while those knowledgeable were 40 (40%).

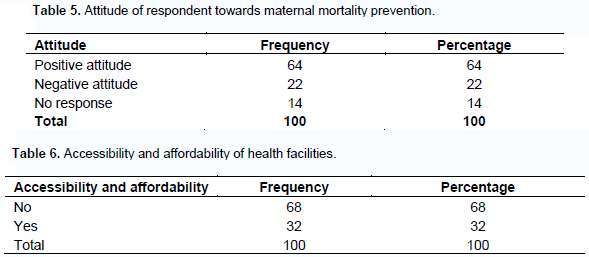
Attitude of respondents on preeclampsia prevention
According to Table 5, 64(64%) had positive attitude towards preeclampsia prevention, 22(22%) had negative attitude towards preeclampsia prevention while 14 (14%) had no response. According to Table 6, majority of respondents (68, 68%) could not access health facilities and services citing the reasons such as unaffordability of health services, long distance to the nearest health facilities, absence of health facilities and services, insecurity while looking for health services and presence of a few health workers in the available health workers, making them to seek other alternatives when they are sick. Only a minority (32, 32%) said that the health facilities were accessible, affordable and efficient.

According to Table 7 on medical history of the respondents during prenatal care, most of the respondents (25%) had increased blood pressure more than 140/90 mmHg, 20% had a complain of severe headache, 14% had blurred vision, 16% had upper abdominal pain, 15% had nausea and vomiting while 10% also had shortness of breath. According to Table 8 on the laboratory investigation results, 48% of respondents had increased proteins in urine (proteinuria), 26% had reduced urine output, 19% had thrombocytopenia, while 7% had impaired liver function. According to Table 9, 39% of the respondents experienced fits/convulsion as a complication of preeclampsia, 24% had pulmonary edema, 20% had kidney failure while 17% had liver failure.
The findings and results obtained in the study is discussed with a view to getting information on hypertension as it relates to pregnant women and the role of medics (Young et al., 2012). According to the study, most of the respondents were aged between 25-34(48%), followed by the age range of 35-44 (12%) and age of between 45-49 (16%), while the young mothers most of the age 15-24 (12%).This shows that most of the respondents, who were in the reproductive stage of life were much more exposed to preeclampsia than any other group (Hollegaard et al., 2013).Thus, there is need to further educate patients about preeclampsia/eclampsia to decrease adverse outcomes associated with this condition (You et al., 2012a, b). Most of respondents were peasants 65 (65%), followed by 19 (19%) who were self-employed and 16 (16%) who were civil servants. This shows that poverty is one cause of high rate of preeclampsia since most of the respondents could not afford to travel or look for health facilities in case of maternal health problems (You et al., 2012b).
According to the study, most of the respondents (48, 48%) covered a long distance of more than 10 km to the nearest health facilities, followed by 36 (36%) who covered 5 to 10 km and lastly 16 (16%) who covered less than 5 km. Distance was also a contributing factor to maternal health problems like preeclampsia since the health facilities were more than 5 km from most of the respondents; therefore most of the residents prefer the alternative to the standard health facilities. This is as a result of the patients' understanding of the implication of preeclampsia/eclampsia if not treated on time (You et al., 2012b; Heidrich et al., 2013; Lo et al., 2013). The findings showed that the majority of the respondents (60, 60%) had primary status of education, 24 (24%) had no formal education, 12 (12%) had secondary form of education and finally 4 (4%) had tertiary education. This shows that they did not have knowledge on the cause and prevention of maternal health problems like preeclampsia or eclampsia and education is also a factor that determines the maternal mortality.
In addition, patients who were exposed to a graphics-based educational tool showed superior pre-eclampsia/eclampsia related knowledge compared to those who were exposed to little or no education (You et al., 2012b; Seely et al., 2015).
From the findings, most of the respondents were young and single (46, 46%), followed by the married who were 17 (17%), the engaged who were 27 (27%), the widowed who were 6 (6%) and those who separated from their partners (4, 4%). This indicates that they could not support themselves in form of financial needs in case of maternal health problems since they were single mothers. Majority of respondents by religion (74, 74%) were Christians while the minorities (26, 26%) were Muslims. Hence, Christians were more exposed to maternal health problems like preeclampsia/eclampsia than any other religion (Ferrer et al., 2000; Solomon and Seely, 2011).
According to the study, the findings showed that respondents' knowledge on maternal mortality due to preeclampsia includes those who had no knowledge (60, 60%) and those who had knowledge (40, 40%). Most of the respondents had no knowledge on maternal mortality due to complications of preeclampsia/eclampsia (Repke et al., 2002). According to the information, 64 (64%) had a positive attitude towards maternal mortality due to preeclampsia prevention, 36(36%) had no response. According to the information, majority of the respondents (68, 68%) could not access the health facilities and health services. while minority 32(32%) said that the health facilities were accessible, affordable and efficient (Heidrich et al., 2013; Garg et al., 2014). Information on medical history during prenatal care showed that about 25% of the respondents had increased blood pressure of more than 140/90 mmHg, severe headache (20%), upper abdominal pain (14%) and only 10% had breath issues among other clinical issues.
This history indicates that the respondents had clinical conditions that could predispose to preeclampsia/eclampsia (Spratling et al., 2014; Imes et al., 2015; Zoet et al., 2015). Laboratory diagnosis of the respondents which revealed increased proteinuria (48%), reduced urine output (26%), thrombocytopenia (19%) and impaired liver function (7%) may be adduced to the presence of biomolecules normally associated with pregnancy-induced hypertension/eclampsia (Mehta et al., 2015), which are potent risk factors. Clinical complications experienced by respondents which included 39% convulsion, 24% pulmonary edema, 20% kidney failure, 17% liver failure are indications of cardiovascular implications of preeclampsia/eclampsia (Seely et al., 2013; Burgess and Founds, 2016).
Majority of respondents, had no knowledge on cause, complication and prevention of preeclampsia/eclampsia and the ignorance could lead to increase in, or could cause maternal mortality. Other problems identified that could lead to preeclampsia among pregnant mothers were poor health education to pregnant mothers since most of them had only primary education, poor roads and insecurity, poverty, long distance to health facilities, harassment by the health workers, unaffordable health services, lack of health workers and lack of education.
1. Government should encourage health education on causes and prevention of the preeclampsia and its complications.
2. Pregnant mothers should take the antenatal care very seriously.
3. Mothers should be encouraged to deliver in the hospital.
4. Eradication of poverty should be carried out by the government.
5. Government should provide enough health facilities
and health workers.
The authors have not declared any conflict of interests.
REFERENCES
|
Aghamohammadi A, Zafari M, Tofighi M (2011). High maternal hemoglobin concentration in first trimester as risk factor for pregnancy induced hypertension. Caspian J. Intern. Med. 2(1):194-197.
|
|
|
|
Burgess A, Founds S (2016). Cardiovascular implications of preeclampsia. Am. J. Matern. Child Nurs. 41(1):8-15.
Crossref
|
|
|
|
|
Daniel WW (1999). Biostatistics: A Foundation for Analysis in the Health Sciences. 7th edition. New York: John Wiley & Sons.
|
|
|
|
|
De Vera MA, Berard A (2012). Antidepressant use during pregnancy and the risk of pregnancy-induced hypertension. Br. J. Clin. Pharmacol. 74(2):362-369.
Crossref
|
|
|
|
|
Ferrer RL, Sibai BM, Mulrow CD (2000). Management of mild chronic hypertension during pregnancy: A review. Obstet. Gynecol. 96:849- 860.
|
|
|
|
|
Garg AX, Nevis IF, McArthur E, Sontrop JM, Koval JJ, Lam NN, Hildebrand AM, Reese PP, Storsley L, Gill JS, Segev DL, Habbous S, Bugeja A, Knoll GA, Dipchand CM, Cuadros M, Lentine KL (2014). "Gestational Hypertension and Preeclampsia in Living Kidney Donors". New Engl. J. Med. 372(45):4790-4793.
|
|
|
|
|
Heidrich MB, Wenzel D, von Kaisenberg CS, Schippert C, von Versen-Hoynck FM (2013). Preeclampsia and long-term risk of cardiovascular disease: what do obstetrician-gynecologists know? - BMC Pregnancy and Childbirth 9:13:61.
|
|
|
|
|
Hollegaard B, Byars SG, Lykke J, Boomsma JJ (2013). Parent-Offspring Conflict and the Persistence of Pregnancy-Induced Hypertension in Modern Humans. PLoS ONE. 8(2):e56821.
Crossref
|
|
|
|
|
Imes CC, Lewis FM, Austin MA, Dougherty CM (2015). My family medical history and me: feasibility results of a cardiovascular risk reduction intervention. Public Health Nurs. 32(3):246-255.
Crossref
|
|
|
|
|
Katon WJ, Russo JE, Melville JL, Katon JG, Gavin AR (2012). Depression in pregnancy is associated with preexisting but not pregnancy-induced hypertension. Gen. Hosp. Psychiatr. 34(1):9-16.
Crossref
|
|
|
|
|
Kintiraki E, Papakatsika S, Kotronis G, Goulis DG, Kotsis V (2015). Pregnancy-Induced hypertension. Hormones 14(2):211-223.
Crossref
|
|
|
|
|
Lo JO, Mission JF, Caughey AB (2013). Hypertensive disease of pregnancy and maternal mortality. Curr. Opin. Obstet. Gynecol. 25(2):124-32.
Crossref
|
|
|
|
|
Mehta PK, Minissian M, Bairey Merz CN (2015). Adverse pregnancy outcomes and cardiovascular risk factor management. Seminars perinatol. 39(4):268-275.
Crossref
|
|
|
|
|
Osungbade KO, Ige OK (2011). Public health perspectives of preeclampsia in developing countries: implication for health system strengthening. J. Pregnancy 481095.
Crossref
|
|
|
|
|
Pieper PG, Lameijer H, Hoendermis ES (2014). Pregnancy and pulmonary hypertension. Best Practice and Research: Clinical Obstetrics Gynaecol. 28(4):579-591.
Crossref
|
|
|
|
|
Repke JT, Power ML, Holzman GB, Suhulklin J (2002). Hypertension in pregnancy and preeclampsia. Knowledge and clinical practice among obstetrician-gynecologists. J. Reprod. Med. 47(6):472-476.
|
|
|
|
|
Sajith M, Nimbargi V, Modi A, Sumariya R (2014). Incidence of pregnancy induced hypertension and prescription pattern of antihypertensive drugs in pregnancy. Int. J. Pharm. Sci. Res. (IJPSR). 5(4):163-170.
|
|
|
|
|
Seely EW, Rich-Edwards J, Lui J, Nicklas JM, Saxena A, Tsigas E, Levkoff SE (2013). Risk of future cardiovascular disease in women with prior preeclampsia: A focus group study. BMC Pregnancy Childbirth 21:13-240.
Crossref
|
|
|
|
|
Seely EW, Tsigas E, Rich-Edwards JW (2015). Preeclampsia and future cardiovascular disease in women: How good are the data and how can we manage our patients? Semin. Perinatol. 39(4):276-283.
Crossref
|
|
|
|
|
Solomon CG, Seely EW (2011). Hypertension in pregnancy. Endocrinol. Metab. Clin. North Am. 10(8):120-125.
Crossref
|
|
|
|
|
Spratling PM, Pryor ER, Moneyham LD, Hodges AL, White-Williams CL, Martin JN Jr (2014). Effect of an educational intervention on cardiovascular disease risk perception among women with preeclampsia. J. Obstet. Gynaecol. Neonatal Nurs. 43(2):179-189.
Crossref
|
|
|
|
|
Steegers EA, von Dadelszen P, Duvekot JJ, Pijnenborg R (2010). Pre-eclampsia. Lancet 376(9741):631-644.
Crossref
|
|
|
|
|
Suzuki Y, Matsuura A, Yamamoto T (2015). Management of pregnancy induced hypertension. Nihon Rinsho. Japanese J. Clin. Med. 73(11):1897-1903.
|
|
|
|
|
van Middendorp D, ten Asbroek A, Bio FY, Edusei A, Meijjer L, Newton S, Agyemang C (2013). Rural and urban differences in blood pressure and pregnancy-induced hypertension among pregnant women in Ghana. Glob. Health 9(1):59.
Crossref
|
|
|
|
|
Veerbeek JH, Hermes W, Breimer AY, Van Rijn BB, Koenen SV, Mol BW, Koster MP (2015). Cardiovascular disease risk factors after early-onset preeclampsia, late-onset preeclampsia, and pregnancy-induced hypertension. Hypertension 65(3):600-606.
Crossref
|
|
|
|
|
Vest AR, Cho LS (2014). Hypertension in pregnancy. Curr. Atheroscler. Rep. 13(6):95-98.
Crossref
|
|
|
|
|
World Health Organization (WHO) (2011). WHO Recommendations for prevention and treatment of pre-eclampsia and eclampsia. Available at:
View
|
|
|
|
|
You WB, Wolf M, Bailey SC, Pandit AU, Waite KR, Sobel RM, Grobman W (2012a). Factors associated with patient understanding of preeclampsia. Hypertens. pregnancy 31(3):341-349.
Crossref
|
|
|
|
|
You WB, Wolf MS, Bailey SC, Grobman WA (2012b). Improving patient understanding of preeclampsia: a randomized controlled trial. Am. J. Obstet. Gynecol. 206(5):431-e1.
Crossref
|
|
|
|
|
Young B, Hacker MR, Rana S (2012). Physicians' knowledge of future vascular disease in women with preeclampsia. Hypertens. pregnancy 31(1):50-58.
Crossref
|
|
|
|
|
Zoet GA, Koster MP, Velthuis BK, de Groot CJ, Maas AH, Fauser BC,Franx A, van Rijn BB (2015). Determinants of future cardiovascular health in women with a history of preeclampsia. Maturitas 82(2):153-161.
Crossref
|
|