ABSTRACT
This study was conducted to evaluate drug resistance profile of Staphylococcus aureus in raw milk, fresh fruit juice and dairy farms settings of Mekelle, Tigray. A cross-sectional study was conducted on the total 258 samples of raw cow milk and fresh fruit juice. Antimicrobial resistance status was also checked for identified S. aureus using various commonly used antimicrobial discs. The overall viable staphylococcal count mean and standard deviation of samples from milk shop, fruit juice and dairy milk were found to be 8.86±107, 7.2 × 107, 8.65±107 cfu/ml, 33.87±106, 6.68±106 and 22.0±106, respectively. Among the total 258 samples, 75 (29.07%) samples were found positive for S. aureus. Proportion of the isolation from milk shop, fruit juice and dairy milk samples were 20 (23.26%), 32 (37.21%) and 23 (26.74%), respectively. Antimicrobial test of the high resistance revealed vancomycin (100%), ampicillin (90.9%). ciprofloxacin (90.9%), ceftaroline (63.6%), penicillin-G (81.8%) and clindamycin (72.7%) whereas they are highly susceptible to some antibiotics like gentamicin (100%), streptomycin (81.8%), norfloxacin (63.6%), chloramphenicol (81.8%), sulfamethoxazole (96%), kanamycin (72.7%), polymixin B (72.7%), erythromycin (72.7%) and tetracycline (81.8); also, some S. aureus also showed multi-drug resistance pattern. The present study, we isolated and determined the drug Resistance profile of S. aruesu in Mekelle city, Northern Ethiopia alarmingly, the S. aureus isolates circulating in the raw cow milk, fresh fruit juice and dairy milk. High level of S. aureus isolation from personnel and equipment besides food samples reveals that the hygiene practice is substandard. Prudent drug use and improved hygienic practice is recommended in the raw cow milk of dairy farms and fresh fruit juice to safeguard the public from the risk of acquiring infections and multiple drug resistance (MDR) pathogenic S. aureus.
Key words: Antibiogram, bacterial load, multiple drug resistance (MDR), Mekelle, Milk, Staphylococcus aureus.
Abbreviation:
AMP, Ampicillin; ANOVA, analysis of variance; CHL, Chloramphenicol; CIP, Ciprofloxacin; ERY, Erythromycin; I, Intermediate; MDR, multiple drug resistance; NSS, normal saline solution; R, resistant; S, Sensitive; SD, standard deviation, O, Observation; STR, Streptomycin; TCY, Tetracycline.
Foods borne illness are public health problem in developed and developing countries. Staphylococcus aureus is among the most significant pathogens causing a wide spectrum of diseases in both humans and animals. In humans, nosocomial and community acquired infections are common (Klotz et al., 2003). Pathogenic strains are usually coagulase-positive and cause disease in their hosts throughout the world. S. aureus is one of the most significant food-borne pathogens (Le Loir et al., 2003). Raw unpasteurized milk may become contaminated with enterotoxigenic coagulase-positive S. aureus either through contact with the cow’s udder during milking or by cross contamination during processing (Normanno et al., 2005, Ekici et al., 2004). Food-borne pathogens are recognized as a major health hazard associated with street foods, the risk being dependent primarily on the type of food and the method of preparation and conservation (CDC, 2011; FAO/WHO, 2005). S. aureus is a gram positive, catalase and coagulase positive microorganism responsible for various foodborne outbreaks. Contamination of food with entero-toxigenic S. aureus causes staphylococcal enterotoxins (SEs) intoxication hence the associated symptoms like vomiting and diarrhea (Veras et al., 2008). In countries where food borne illness were investigated and documented, the relative importance of pathogens like S. aureus, Campylobacter, Escherichia coli and Salmonella species were recorded as a major cause (WHO, 2004). The ability of these microorganisms to survive under adverse conditions and to grow in the presence of low levels of nutrients and at suboptimal temperatures and pH values presents a formidable challenge to the agricultural and food processing industries.
The continued prominence of raw meats, eggs, dairy products, vegetable sprouts, fresh fruits and fruit juices as the principal vehicles of human foodborne diseases poses a major challenge to coordinate sectorial control efforts within each industry (Knife and Abera, 2007). Studies conducted in different parts of Ethiopia also showed the poor sanitary conditions of catering establishments and presence of pathogenic organisms (Knife and Abera 2007; Mekonnen et al., 2012). In addition to toxic effect of food borne microbial pathogens, antibiotic resistance remains a major challenge in human and animal health (Shekh et al., 2013). Food contamination with antibiotic-resistant bacteria can therefore be a major threat to public health, as the antibiotic resistance determinants can be transferred to other bacteria of human and animals, thereby has significant public health implications by increasing the number of food-borne illnesses and the potential for treatment failure (Adesiji et al., 2011). Studying antimicrobial resistance in humans and animals is important for detecting changing patterns of resistance, implementing control measures on the use of antimicrobial agents and preventing the spread of multidrug-resistant strains of bacteria. Up to now, many researchers have focused on the spread of resistant S. aureus in clinical settings (Ateba et al., 2010; Addo et al., 2011). However, limited number of investigations has been studied about the presence of antimicrobial resistance in food animals in Ethiopia (Mekonnen et al., 2005; Hundera et al., 2005). So far, there are no studies conducted on the burden and drug sensitivity profile of S. aureus in Mekelle city, Northern Ethiopia. In this study, S. aureus was isolated and the drug Resistance profile was determined.
Study area
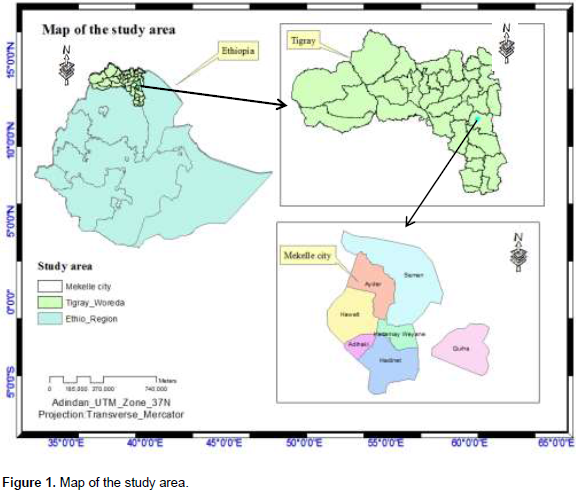
The study was conducted from October 2016 to June 2017 in Mekelle city. Mekelle is the capital city of Tigray Regional State located at about 783 km away north of Addis Ababa, Capital city of the Federal Democratic Republic of Ethiopia at geographical coordination of 39°28` East longitude and 13°32` North latitude. The average altitude of the city is 2300 m.a.s.l. with a mean annual rainfall and average annual temperature of 629 mm and 22°C, respectively (TBA, 2017). The population of the city is 406,338 (195, 605 male and 210,733 female) (TBA, 2017). The city has seven sub-cities and 33 Kebelles where over 139 juice houses, 48 dairy farms and 123 milk shops (street vender or retailer shops) are inhabited. Besides, the city possesses an extensive public transport network and active urban-rural exchange of goods with about 30,000 micro and small enterprises (Bryant, 2017).
Study design
A cross-sectional survey was conducted from October 2016 to June 2017 on raw cow milk and fresh fruit juice samples collected from different sources of raw milk shops and dairy milk supply centers, and juice houses in Mekelle. Purposive sampling technique was employed.
Sampling technique and collection
A total of 258 food samples were collected among which 172 are milk samples (86 from milk shops, 86 from dairy farms) and the remaining 86 are fresh juice samples (from 86 juice houses) in the seven sub-cities of Mekelle city. Samples were collected according to standards described by Oyeleke and Manga (2008). After aseptic collection, samples were labeled and packed with sterile bottles and transported with an ice box to Mekelle University, College of Veterinary Medicine, Microbiology and Public health laboratories for bacterial isolation and characterization. Samples were processed immediately for bacterial identification to species level using culture media and then isolates were kept in refrigerator at 4°C until microbial characterization with regular sub-culturing described (Oyeleke and Manga, 2008).
Enumeration of total viable
One milliliter and gram of raw milk and fruit juice samples respectively were homogenized into 9 ml of serial peptone water/NSS and 10 g/1 g of each food item was weighed out and homogenized into 90 ml/9 ml of sterile distilled deionized water. Then, serial dilutions were prepared. From the 10-fold dilutions of the homogenates; 1 ml of 10-4, 10-5 and 10-6 dilutions were cultured in replicate on standard plate count agar (Hi Media, India), using the pour plate method. The plates were then incubated at 37°C for 24 – 48 h. At the end of the incubation period, colonies were counted using the illuminated colony counter. The counts for each plate were expressed as colony forming unit of the suspension (cfu/g) (Fawole and Oso, 2001). In order to determine the presence of S. aureus, 0.1 ml of samples from each dilution was introduced onto the Baird Parker agar (Oxorid). The plates were incubated at 37°C for 24 h. All the isolates were subjected to morphological and biochemical confirmation according to the prescribed method (Fawole and Oso, 2001).
Isolation and identification of S. aureus
About 10 ml of each raw cow milk and fresh fruit juice sample was suspended in 90 ml of Brain heart infusion broth supplemented with NaCl (6.5%) and incubated at 37°C for 24 h. A sterile loopful of the broth inoculum was streaked onto Baird Parker agar and incubated at 37°C for 24 h. Colonies that appeared black or greyish-black were Gram-stained and subjected to biochemical tests. Gram positive cocci that occurred singly and in pairs, tetrads, short chains and irregular grape-like clusters were suggestive of S. aureus. Conventional biochemical tests carried out for presumptive identification of S. aureus isolates included gram staining, catalase, coagulase, 5 % sheep blood agar, pigmentation (Mannitol salt agar) and DNase activity (McFaddin, 2000).
Antimicrobial susceptibility test
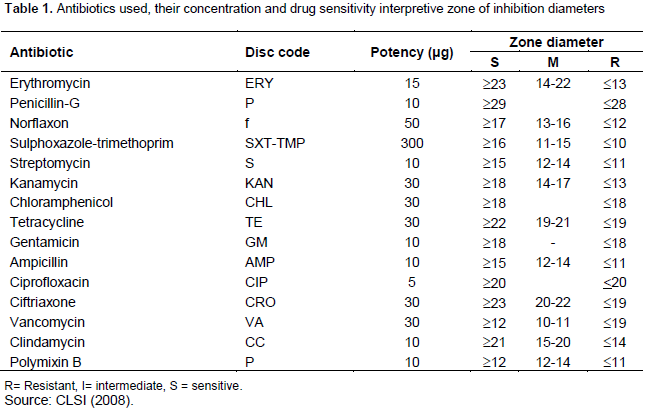
Antimicrobial susceptibility test, through Kirby diffusion test, was performed for all S. aureus isolates following the protocol of CLSI (2008). For susceptibility test, a pure culture of all S. aureus were taken and transferred to a tube containing 5 ml of sterile normal saline and mixed gently to make homogenous suspension which was adjusted to a turbidity equivalent to a 0.5 Mc Far land standard as measured by turbidity meter. The bacterial suspension was inoculated onto Muller–Hinton agar (Oxorid, UK) with the sterile swab to cover the whole surface of the agar. The inoculated plates were left at room temperature to dry. Before using the antimicrobial disks, they were kept at room temperature for 1 h and then dispended on the surface of media. Following this, the plates were incubated aerobically at 37°C for 24 h (CLIS, 2012). The diameters of the zone of inhibition around the disks were measured to the nearest millimeter using calibrated rulers, and the isolates were classified as susceptible, intermediate and resistant according to the interpretative accordance with the guidelines of (CLSI, 2008) as indicated in Table 1.
Data management and analysis
All data were checked against the standards and methods were used to perform the study. Data was entered in Microsoft Excel spreadsheet and analyzed using STATA Version 12. Descriptive statistics such as means, percentage and frequencies were computed to report desired outputs. The antimicrobial resistance test was analyzed using WHONET software version 5 statistical package (http://www.who.int/medicines/areas/rational_use/AMR_WHONET_SOFTWARE/en/). Analysis of Variance (ANOVA) was used to test the significant difference at p < 0.05.
Enumeration of total viable
The overall mean viable bacterial count recorded was 8.24 x 107. The individual sample type mean viable count and standard deviation of milk shop, fruit juice and dairy milk is indicated in Table 2.

Isolation and Identification of organism
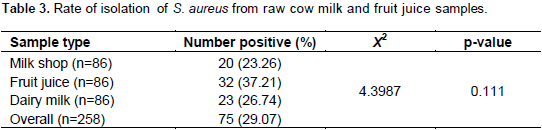
Among the total 258 raw cow milk and fruit juice samples collected from different sources of Mekelle sub city, 75 (29.07%) samples were found positive for S. aureus. Proportion of the isolation from milk shop, fruit juice and dairy milk samples is described (Table 3). A statistically significant difference (χ2=4.3987, P-value =0.111) was recorded among samples from the three sites (Table 3 and Figure 1).

Antimicrobial susceptibility profile of S. aureus
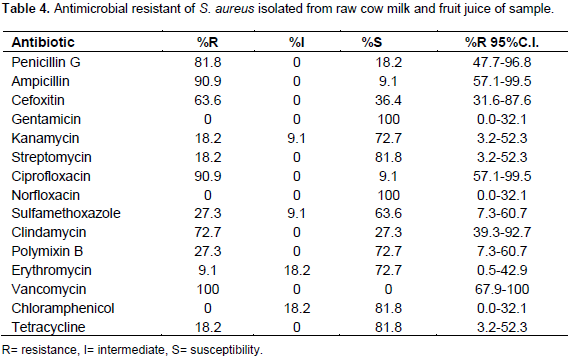
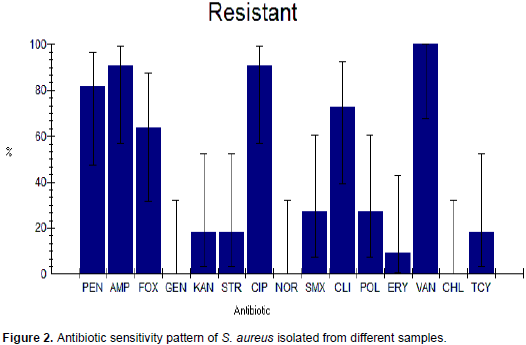
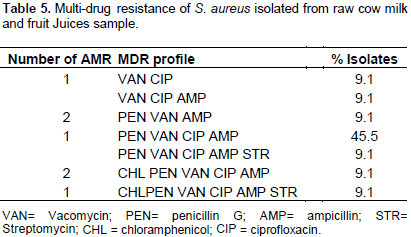
The antimicrobial resistance profile of the bacterial isolates from raw cow milk and fruit juice samples are summarized in Table 3. S. aureus showed high resistance to antibiotics like, vancomycin (100%), ampicillin (90.9%). ciprofloxacin (90.9%), ceftaroline (63.6%), pencillin-G (81.8%) and clindamycin (72.7%) whereas it was highly susceptible to some antibiotics like, gentamicin (100%), streptomycin (81.8%), norfloxacin (63.6%), chloramphenicol (81.8%), sulfamethoxazole (96%), kanamycin (72.7%), polymixin B (72.7%), erythromycin (72.7%) and tetracycline (81.8) (Table 4 and Figure 2). The multi-drug resistance pattern of the bacterial S. aureus isolates is presented in Table 5. In general, antimicrobial susceptibility test revealed that gentamicin, streptomycin, norfloxacin, chloramphenicol, sulfamethoxazole, kanamycin, polymixin B, erythromycin, and tetracyclin were the antimicrobials indicated as active against S. aureus isolated from this study. A total of 10 multiple drug resistance patterns were observed. The highest multiple drug resistance (MDR) noted was PEN, VAN, CIP and AMP (45.5%). The maximum multiple drug resistance registered was resistant to three and four antibiotics with the combination PEN, VAN, CIP and AMP.
The current finding indicates that samples from milk shop, fruit juice and dairy milk were found with a viable staphylococcal count load of 8.86 × 107, 7.2 × 107 and 8.65 × 107 cfu/ml respectively with an overall mean viable bacterial count of 8.24 × 107cfu/ml. The highest mean value of microbial load (8.86 × 107 cfu/ml) was found from milk shop samples. The current study was found with higher viable staphylococcal count than previous reports such as viable bacterial count from raw cow milk and fresh fruit juice samples in 6.0 × 103 cfu/ml to 2.5 × 105 cfu/ml of (Lucky et al., 2016) in Bangladesh, 1.4 × 104 cfu/ ml (Tasnim, 2016) in Dhaka city; Staphylococcal count was from fresh vended fruit juices. In the present study, out of 258 samples, 75 (29.07%) samples were found to be positive for S. aureus of which 20 (23.26%) were from milk shop, 32 (37.21%) from fruit juice and 23 (26.74%) from dairy milk. The result shows a high contamination rate, which might be attributed to poor hygeinic sanitation and handling improper. Statistically significant difference (P< 0.05) among the sample types in the prevalence of S. aureus was recorded. A similar report was also made by previous researchers (Abebe et al., 2013; Reta et al., 2016) that S. aureus was 15.5 and 24.2% in raw milk samples respectively in Ethiopia and in the other parts of the world which is contrary to this; different literatures revealed a very significant isolation rate of S. aureus from raw milk samples (Olatunji et al., 2009; Pourhassan and Taravat-Najafabadi, 2011; Mohanty et al., 2013; Sanaa et al., 2005).
The present overall isolation rate in raw cow milk products was 29.07% which seems to be higher than the findings of 6.25% by Thaker et al. (2013), 17% in Egypt (El-Gedawy et al., 2014), 18.2% in Turkey (Ekici et al., 2004), 20.8% in Turkey (Aydin et al., 2011) and 21% in Iran (Ahmadi et al., 2009); were previously reported in milk samples collected from dairy farms. The present finding was much higher compared to the finding reported previously (Santana et al., 2010; Ekici et al., 2004) which found 17.39 and 18.18%, respectively; 4 (8%) of pasteurized milk samples, 9 (18%) of traditional butter samples and 12 (24%) of traditional cheese samples (Mirzaei et al., 2011) in Sarab whereas the new finding was much lower compared to the finding reported; 40% (Zakary et al., 2011), 22.5% (Hamid et al., 2017), 61.70% (Lingathurai and Vellathurai, 2011) and 44% (Mirzaei et al., 2011) from raw milk samples in Sarab. The variation could be due to the reason that even when drawn under aseptic condition, milk always contains microorganisms which are derived from the milk ducts in the udder. In addition, contaminants coming from milking utensils, human handlers, unclean environmental conditions and poor udder preparation might expose raw milk to bacterial contamination.
Moreover, the present study showed the resistance of S. aureus to vancomycin (100%), ampicillin (90.9%), ciprofloxacin (90.9%), ceftaroline (63.6%), pencillin-G (81.8%) and clindamycin (72.7%) whereas was highly susceptible to some antibiotics like, gentamicin (100%), streptomycin (81.8%), norfloxacin (63.6%), chloramphenicol (81.8%), sulfamethoxazole (96%), kanamycin (72.7%), polymixin B (72.7%), erythromycin (72.7%) and tetracycline (81.8) (Table 4). Similarly, the present investigation indicated that the resistance pattern of penicillin was found to be 93.1% by Melese et al. (2016) which is similar to the finding (87.2 %) of Tariku et al. (2011) in Ethiopia, 80% in Sweden (Landin, 2006), 57% in Iran (Gooraninejad et al., 2007) and 50% in Finland (Myllys et al., 1998). This is in contrast to findings observed by (Adesiyun, 1994) who reported 23% of resistance to penicillin-G in West India. The highest drug resistance recorded in the current study migh be due to high antimicrobial use in dairy farms and individual cows, to treat various diseases affecting the dairy sector. Similarly, several studies have indicated that S. aureus isolated from raw milk showed high resistance to vancomycin, ampicillin, ciprofloxacin, penicillin-G followed by ciprofloxacin and clindamycin thus indicating the safety of food products. However, few numbers of isolates exhibited resistance towards ampicillin (Thaker et al., 2013).
Antibiotic resistance development among the bacteria poses a problem of concern. Effectiveness of current treatments and ability to control infectious diseases in both animals and humans may become hazardous. Different researchers reported antimicrobial resistant S. aureus isolates of raw milk in their previous studies from Ethiopia. Reports from other researchers had also indicated S. aureus isolates resistance to vancomycin (100%), ampicillin (90.9%), ciprofloxacin (90.9%), ceftaroline (63.6%), penicillin-G (81.8%) and clindamycin (72.7%). Similar result was most frequently observed for penicillin (100%), ampicillin (100%), followed by erythromycin (95.7%) (Wang et al., 2014) in China, penicillin (100%), ampicillin (96%), amoxicillin (92%), and trimethoprim- sulphamethoxazole (88%) (Beyene, 2016) in Ethiopia, whereas the percent were found higher compared to what was reported by Hamid et al. (2017) of 94.4, 83.3 and 50% resistance for penicillin, ampicillin and ceftriaxone, respectively of S. aureus isolates with particular emphasis on penicillin G. The present observation agrees with preliminary finding conducted by Reta et al. (2016) of 93.1%. This is in accordance with the findings of Tariku et al. (2011) who reported resistance of S. aureus to chloramphenicol (16%), vancomycin (3%) it lower with compare the present finding while as (Khakpoor et al., 2011) in other study reported that all isolate of S. aureus from mastitis cattle were resistant to penicillin and 83.3% resistance to ampicillin in this study is much higher than that of 41.44% as reported by (Mubarack et al ., 2012) and lower as compared to 100% resistance reported by (Khakpoor et al., 2011).
The current study was highly susceptible to some antibiotics like, gentamicin (100%), streptomycin (81.8%), norfloxacin (63.6%), chloramphenicol (81.8%), sulfamethoxazole (96%), kanamycin (72.7%), polymixin B (72.7%), erythromycin (72.7%) and tetracycline (81.8); similar results were found for chloramphenicol, streptomycin and gentamycin (100, 94, and 90%), respectively by Beyene (2016) in Ethiopia but disagree with the observation made by Kassaify et al. (2013) in the case of streptomycin (95%), but it disagree with the observation made by Tariku et al. (2011) in the case of tetracycline (0%) and clindamycin (4%) in dairy farms in Jimma town, cefoxitin (100%) and clindamycin (each 100%) (Wang et al., 2014) in China. The probable explanation could be that S. aureus strains have the capacity to change their resistance behavior to the exposed antimicrobials. The emergence degree of resistance to many drugs represents public health hazard due to the fact that food borne outbreaks would be difficult to treat and this pool of MDR S. aureus in food supply represents a reservoir for communicable resistant genes. The reason for the existence of antimicrobial resistant salmonella isolates could be due to the indiscriminate use of antimicrobials, self-medication, administration of sub therapeutic dose of antimicrobials to livestock for prophylactic purpose (Szyfers and Acha, 2001) and limited updating of the long used drug groups. Hence, due to the relatively limited access and high price to get the newly developed cephalosporin and quinolone drugs, the reports of prevalence of antimicrobial-resistant to relatively low-priced and regularly available antibiotics are alarming for a low-income society living in most developing countries, like Ethiopia.
The current study showed insights into the magnitude and incidence of S. aureus from raw cow milk and fresh fruit juice samples. The study revealed the development of antibiotic resistant against S. aureus which could pose serious threat for consumers as well as for health professionals in the study area. Hence, attention should be given to proper handling of the food items, and using recent antibiotics in the treatment of diseases both in humans and animals.
The authors have not declared any conflict of interests.
REFERENCES
|
Abebe M, Daniel A, Yimtubezinash W, Genene T (2013). Identification and antimicrobial susceptibility of S. aureus isolated from milk samples of dairy cows and nasal swabs of farm workers in selected dairy farms around Addis Ababa, Ethiopia. Afr. J. Microbiol. Res. 7(27):3501-3510.
|
|
|
|
Addo KK, Mensah GI, Aning KG, Nartey N, Nipah GK, Bonsu C, Akyeh ML, Smits HL (2011). Microbiological quality and antibiotic residues in informally marketed raw cow milk within the coastal savannah zone of Ghana. Trop. Med. Int. Health 16(2):227-32.
Crossref
|
|
|
|
|
Adesiji YO, Alli OT, Adekanle MA, Jolayemi JB (2011). Prevalence of Arcobacter, Escherichia coli, Staphylococcus aureus and Salmonella species in Retail Raw Chicken, Pork, Beef and Goat meat in Osogbo, Nigeria. J. Biomed. Res. 3(1):8-12
Crossref
|
|
|
|
|
Adesiyun A (1994). Characteristics of S. aureus strains isolated from bovine mastitic milk: Bacteriophage and antimicrobial agent susceptibility and enterotoxigenecity. J. Vet. Med. 42:129-39.
Crossref
|
|
|
|
|
Ahmadi M, Rohani SMR, Ayremlou N (2009). Detection of Staphylococcus aureus in milk by PCR. Comp. Clin. Pathol. 19(1):91-94.
Crossref
|
|
|
|
|
Ateba CN, Mbewe M, Moneoang MS, Bezuidenhout CC (2010) Antibiotic-resistant Staphylococcus aureus isolated from milk in the Mafikeng Area, North West province. South Afr. J. Sci. 106:1-6.
Crossref
|
|
|
|
|
Aydin A, Sudagidan M, Muratoglu K (2011). Prevalence of staphylococcal enterotoxins, toxin genes and genetic-relatedness of foodborne Staphylococcus aureus strains isolated in the Marmara Region of Turkey. Int. J. Food Microbiol. 148(2):99-106.
Crossref
|
|
|
|
|
Beyene GF (2016). Antimicrobial Susceptibility of Staphylococcus aureus in Cow Milk, Afar Ethiopia Int. J. Modern Chem. Appl. Sci. 3(1):280-283.
|
|
|
|
|
Bryant C. (2017). Investment opportunities in Mekelle, Tigray state, Ethiopia.
|
|
|
|
|
Centers for Disease Control and Prevention (CDC) (2011). Estimates of Foodborne Illness in the United States. Available at:
View.
|
|
|
|
|
Clinical and Laboratory Standards Institute (CLSI) (2008). Performance standards for antimicrobial disk and dilution susceptibility tests for bacteria isolated from animals third edition. Approved standard M31-A3. CLSI, Wayne, PA.
|
|
|
|
|
Clinical and Laboratory Standards Institute (CLSI) (2012). Performance standards for antimicrobial susceptibility testing; twenty second informational supplements. CLIS document M100-S22 Wayne PA.
|
|
|
|
|
Ekici K, Bozkurt H, Isleyici O (2004). Isolation of some pathogens from raw milk of different milk animals. Pak. J. Nutr. 3(3):161-162.
Crossref
|
|
|
|
|
El-Gedawy AA, Ahmed HA Awadallah MA (2014). Occurrence and molecular characterization of some zoonotic bacteria in bovine milk, milking equipments and humans in dairy farms, Sharkia, Egypt Int. Food Res. J. 21(5):1813-1823.
|
|
|
|
|
FAO/WHO (2005). Informal food distribution sector in Africa (street foods): importance and challenges CAF 05/4.
|
|
|
|
|
Fawole MO, Oso BA (2001) Laboratory manual of Microbiology: Revised edition, Spectrum Books Ltd, Ibadan. P 127.
|
|
|
|
|
Gooraninejad S, Ghorbanpoor M, Salati AP (2007). Antibiotic Susceptibility of Staphylococci isolated from bovine sub-clinical mastitis. Pak. J. Biol. Sci. 10:2781-2783.
Crossref
|
|
|
|
|
Hamid S, Bhat MA, Mir IA, Taku A, Badroo GA, Nazki S, Malik A (2017). Phenotypic and genotypic characterization of methicillin-resistant Staphylococcus aureus from bovine mastitis. Vet. World 10(3):363-367.
Crossref
|
|
|
|
|
Hundera S, Ademe Z, Sintayehu A (2005). Dairy cattle mastitis in and around Sebeta, Ethiopia. J. Appl. Res. Vet. Med. 3:1525-1530.
|
|
|
|
|
Khakpoor M, Safarmashaei S, Jafary R (2011). Study of milk extracted from cows related to Staphylococcus aureus by culturing and PCR. Global 7(6):572-575.
|
|
|
|
|
Klotz M, Opper S, Heeg K, Zimmermann S (2003). Detection of Staphylococcus aureus enterotoxins A to D by real-time fluorescence PCR assay. J. Clin. Microbiol. 41(10):4683-4687.
Crossref
|
|
|
|
|
Knife Z, Abera K (2007). Sanitary conditions of food establishments in Mekelle town, Tigray, north Ethiopia. J. Health Dev. 21(1):3–11.
|
|
|
|
|
Landin H (2006). Treatment of mastitis in Swedish dairy production (in Swedish with English summary). Svensk Veterinärtidning 58:19-25.
|
|
|
|
|
Le Loir Y, Baron F, Gautier M (2003). Staphylococcus aureus and food poisoning. Genet. Mol. Res. 2(1):63-76.
|
|
|
|
|
Lingathurai S, Vellathurai P (2011). Bacteriological quality and safety of raw cow milk in Madurai, South India. Webmed Center Microbiol. 1:1-10.
|
|
|
|
|
Lucky NA, Nur IT, Ahmed T (2016). Microbiological quality assessment for drug resistant pathogenic microorganisms from the fresh vended fruit juices in Bangladesh, Stamford J. Microbiol. 6(1):7-10.
|
|
|
|
|
McFaddin JF (2000) Biochemical Tests for the Identification of Medical Bacteria, 3rd. Lippincott Williams & Wilkins, Philadelphia. pp. 94-95.
|
|
|
|
|
Mekonnen H, Habtamu T, Kelali A (2012). Contamination of "raw" and "ready-to-eat" foods and their public health risks in Mekelle City, Ethiopia. ISABB J. Food Agric. Sci. 2(2):20-29.
|
|
|
|
|
Mekonnen H, Workineh S, Bayleyegne M, Moges A, Tadele K (2005). Antimicrobial susceptibility profile of mastitis isolates from cows in three major Ethiopian dairies. Revue de médecine vétérinaire 176:391-394
|
|
|
|
|
Mirzaei H, Tofighi A, Karimi Sarabi, Mahdi Farajli (2011). Prevalence of Methicillin-Resistant Staphylococcus aureus in Raw Milk and Dairy Products in Sarab by Culture and PCR Techniques. J. Anim. Vet. Adv, 10(23):3107-11.
|
|
|
|
|
Mohanty NN, Das P, Pany SS, Sarangi LN, Ranabijuli S, Panda HK (2013). Isolation and antibiogram of Staphylococcus, Streptococcus and E. coli isolates from clinical and subclinical cases of bovine mastitis. Vet. World 6(10):739-743.
Crossref
|
|
|
|
|
Mubarack HM, Doss A, Vijayasanthi M, Venkataswamy R (2012). Antimicrobial drug susceptibility of Staphylococcus aureus from subclinical bovine mastitis in Coimbatore, Tamil Nadu, South India. Vet. World 5(6):352-355.
Crossref
|
|
|
|
|
Myllys V, Asplund K, Brofeld E, Hirevela-Koski V, Honkanen-Buzalski T (1998). Bovine Mastitis in Filand in 1988 and 1995. Changes in Prevalence and Antimicrobial resistance. Acta Vet. Scand. 39:119–26.
|
|
|
|
|
Normanno G, Firinu A, Virgilio S, Mula G, Dambrosio A, Poggiu A, Decastelli L, Mioni R, Scuota S, Bolzoni G, Giannatale EDi, Salinetti AP, Salandra GLa, Bartoli M, Zuccon F, Pirino T, Sias S, Parisi A, Quaglia NC, Celano GV (2005). Coagulase-positive staphylococci and Staphylococcus aureus in food products marketed in Italy. J. Food Microbiol. 98:73-79.
Crossref
|
|
|
|
|
Olatunji EA, Ahmed I, Ijah UJ (2009). Evaluation of microbial qualities of skimmed milk (nono) in Nasarawa State, Nigeria. Proceeding of the 14th Annual Conf. of Ani.Sc. Asso. Of Nig. (ASAN) LAUTECH Ogbomoso, Sept. 14th-17th.
|
|
|
|
|
Oyeleke SB, Manga SB (2008). Essentials of laboratory practical are in microbiology, to best publisher Minna, Nigeria. pp. 36-75.
|
|
|
|
|
Pourhassan M, Taravat-Najafabadi ART (2011). The spatial distribution of bacterial pathogens in raw milk consumption on Malayer City, Iran. Shiraz Med. J. 12:2-10.
|
|
|
|
|
Reta MA, Bereda TW, Alemu AN (2016). Bacterial contaminations of raw cow's milk consumed at Jigjiga City of Somali Regional State, Eastern Ethiopia. Int. J. Food Contamin. 3:4.
Crossref
|
|
|
|
|
Sanaa OY, Nazik EA, Ibtisam EM, Zubeir EL (2005). Incidence of Some Potential Pathogens in Raw Milk in Khartoum North (Sudan) and Their Susceptibility to Antimicrobial Agents. J. Anim. Vet. Dev. 4(3):356-359.
|
|
|
|
|
Santana EHW, Cunha MLRS, Oliveira TCRM, Moraes LB, Alegro LCA (2010). Assessment of the risk of raw milk consumption related to staphylococcal food poisoing. Ciência Animal Brasileira pp. 643-652.
|
|
|
|
|
Shekh CS, Deshmukh VV, Waghamare RN, Markandeya NM, Vaidya MS (2013). Isolation of pathogenic Escherichia coli from buffalo meat sold in Parbhani city, Maharashtra, India. Vet. World 6(5):277-279
Crossref
|
|
|
|
|
Szyfres B, Acha PN (2001). Zoonoses and communicable diseases common to man and animals: In Bacteriosis and Mycosis (3rd ed.), Washington DC: Pan Am. Health Organ. 1:233-246.
|
|
|
|
|
Tariku S, Jemal H, Molalegne B (2011). Prevalence and susceptibility assay of Staphylococcus aureus isolated from bovine mastitis in dairy farms in Jimma town South West Ethiopia. J. Anim. Vet. Adv. 10:745-749.
Crossref
|
|
|
|
|
Tasnim M (2016). Isolation and identification of microbes from various fruit juices made and sold for immediate consumption at home and in the market of Dhaka city, MSc thesis.
|
|
|
|
|
Tigray bearou of administration (TBA) (2017). Tigray bearou of administration population census commission. Summary and statistical report of population and housing. Tigray bearou of Adiminstration.
|
|
|
|
|
Thaker HC, Brahmbhatt MN, Nayak JB (2013). Isolation and identification of Staphylococcus aureus from milk and milk products and their drug resistance patterns in Anand, Gujarat. Vet. World 6(1):10-13.
Crossref
|
|
|
|
|
Veras JF, Carmo LS, Tong LC, Shop JW, Cummings C, Santos DA, Cerqueira MMOP, Cantini A, Nicoli JR, Jett M (2008). A study of the enterotoxigenicity of coagulase negative and coagulase positive staphylococcal isolates from food poisoning outbreaks in Minas Gerais Brazil. J. Infect. Dis. 12:410-415.
Crossref
|
|
|
|
|
Wang X, Li G, Xia X, Yang B, Xi M, Meng J (2014). Antimicrobial susceptibility and molecular typing of methicillin-resistant staphylococcus aureus in retail foods in Shaanxi, China. Foodborne Pathog. Dis. 11(4):281-286.
Crossref
|
|
|
|
|
World Health Organization (WHO) (2004). Regional office for Africa developing and maintaining food safety control systems for Africa current status and prospects for change, Second FAO/WHO Global Forum of Food Safety Regulators. Bangkok, Thailand. pp. 12-14.
|
|
|
|
|
Zakary EM, Nassif MZ, Mohammed GMO (2011). Detection of Staphylococcus aureus in Bovine Milk and its Product by Real Time PCR Assay. Glob. J. Biotechinol. Biochem. 6(4):171-177.
|
|
|
|
|
Zeina K, Pamela AK, Fawwak S (2013). Quantification of Antibiotic Residues and Determination of Antimicrobial Resistance Profiles of Microorganisms Isolated from Bovine Milk in Lebanon. Food Nutr. Sci. 4:1-9.
Crossref
|
|